Knee pain… and a 30 year history of migraines
The patient: Mrs Lovely Person, now age 39, recently stopped working, two young children and a beautiful husband.
Background: As is often the case, in April 2009 this patient presented with one condition and ended up being treated for two. During her treatments for a knee injury it emerged that she had been a long term migraine sufferer since the age of 10. The possible genesis was a road traffic accident where she was a passenger in a builder’s van. The van was parked and struck from behind by another vehicle. A builder’s trellis, in the back flew forward and struck her on the back of the neck.
Clinical highlights: The migraines were monthly, left sided, in the form of pain through the eye, lasting three to four days ending with nausea and vomiting which usually marked the end of the episode. On the occasions that she had been in my practice with a migraine her left pupil would be dilated. Palpation of the cervical spine demonstrated significant “Old Tissue Thickening” of the left C2/3 Zygapophysial joint. Pressure here created a sensation of nausea and pain through the left eye.
Treatment: Manual therapy for the issues in the tissues and pain education for the central components. The patient was ‘on side’ concerning the knowledge. Over a two-year period of diminishing attendance we achieved an enduring, migraine free life style.
The migraines return
Clinical Highlights Autumn 2015: In autumn 2014, the migraines slowly returned. The patient waited one year hoping that the episodes would pass then finally surrendered for treatment. A similar pattern as before. Again positive palpation findings of the left C2/3 zygapophysial joint. Again pressure here caused a strong sensation of nausea and pain through the left eye. Positive left ULNT 1 creating a pupil response on the left. Decision taken to stop working to be with her children. Generally happy with life and enjoying a good marriage.
Treatment: In addition to the manual therapy and pain science education, introduction of the Protectometer. Again the pattern of and severity of the migraines is improving.
The latest migraine packs a surprise
However, her last migraine attack created a “black eye” response:
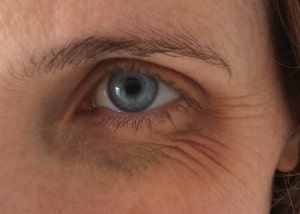
This patient is a credible witness and assures me that absolutely no physical insult to the region has occurred. She is not on blood thinners and has not been rubbing the eye to relieve the pain.
I leave you to ponder this
Is this a powerful example of the brain not needing an extrinsic insult to respond? Was the shooting pain through the eye, during the migraine attack sufficient for the brain to believe that the eye was insulted? I leave you to ponder but I know what I think…
-David Bolton
London
David Bolton, MCSP MMACP MSOM, has over 40 years of clinical experience in the field of neuromusculoskeletal medicine and is a long time NOI faculty member. At Limbus in Chelsea Harbour, David specialises in treating difficult pain states with a biopsychosocial treatment philosophy.
![aussie_tour_banner_2016[1]](https://noigroup.com/wp-content/uploads/2020/11/aussie_tour_banner_20161.jpg)
We’re hitting the road and taking our NOI courses right across this great southern land:
Noosa 17 – 19 June Explain Pain and Graded Motor Imagery (Both courses SOLD OUT)
Wagga Wagga 16-17 July Explain Pain
Perth 15 – 17 October Explain Pain and Graded Motor Imagery

EP3 events have sold out three years running in Australia, and we are super excited to be bringing this unique format to the United States in late 2016 with Lorimer Moseley, Mark Jensen, David Butler, and few NOI surprises.
EP3 EAST Philadelphia, December 2, 3, 4 2016
EP3 WEST Seattle, December 9, 10, 11 2016
To register your interest, contact NOI USA:
p (610) 664-4465
e noius@noigroup.com


Hi David
A really powerful piece, and an eloquent reminder that those who understand pain and have the courage to Explain Pain, are also able to still place ‘hands on’ and use skilled manual handling to help effect change.
Tim
Hi David,
I agree with you and as an aside, I found it interesting that you noticed the upper limb neurodynamic test evoked a pupillary response in the patient – perhaps a flare early on in the test and then the pupil may have stayed dilated for a bit? This may hint at some issue along the oculosympathetic pathway involving the trigeminal nerve and the ophthalmic branch with a neurogenic inflammatory response in the eyelids.
David