If you live with chronic pain, you’ve probably been told – at least once – that stress makes it worse. And you probably already know that. What you might not have been told is why, or quite how deep that connection runs. The relationship between stress and chronic pain isn’t incidental. Stress influences your nervous system, your hormones, your immune function, and how pain is experienced. This Stress Awareness Month, April 2026, we want to walk you through what’s actually happening in your body, because understanding it changes how you relate to it.
What is stress, really?
Stress is one of those words everyone uses, but few people stop to define. Robert Sapolsky, one of the most readable scientists writing on stress, puts it plainly – ‘A stressor is anything that knocks you out of balance, and the stress response is what your body does to restore it.’
At its core, it’s your body’s response to a real or perceived threat to its balance. It can arise when life feels unpredictable, uncontrollable, or overwhelming – whether that comes from physical injury, a difficult conversation, financial pressure, or even your own thoughts about pain. What makes this worth sitting with is that your body doesn’t always distinguish between a physical danger and a psychological one. As Sapolsky observes, we humans are smart enough to generate stress responses purely from our own thoughts – and those responses are just as real and biologically powerful as any physical threat. Both can activate the same systems. Both can feed into how pain is experienced.
Your body is doing exactly what it has evolved to do
When stress hits, your body responds fast. Energy mobilises. Heart rate rises. Breathing quickens. Attention sharpens. Many systems adapt toward a state associated with protection. In the right context, this is extraordinary. The trouble is, it likely evolved for short-term, physical threats – not the ongoing, invisible pressures that make up so much of modern life. And certainly not the ongoing stress associated with persistent pain states.
When stress doesn’t switch off
The system evolved to deal with short-term challenges, not problems that persist. When your stress response stays active for days or weeks rather than minutes, the body shifts resource allocation – dialling down digestion, tissue repair, and immune function in favour of staying ready to act. It’s a sensible short-term strategy. Over time, it becomes a costly one. As Sapolsky puts it, we so often activate a physiological system built for acute physical emergencies, but run it for months on end – worrying about mortgages, relationships, and the pain that won’t go away, contributing to fatigue, disrupted sleep, increased inflammation, and changes in how nociceptive information is processed and weighed.
This helps explain why stress is so often intertwined with chronic pain conditions.
Why stress and pain keep feeding each other
In the short term, stress can temporarily reduce pain intensity – a useful adaptation for emergencies. But when stress becomes ongoing, it tends to do the opposite.
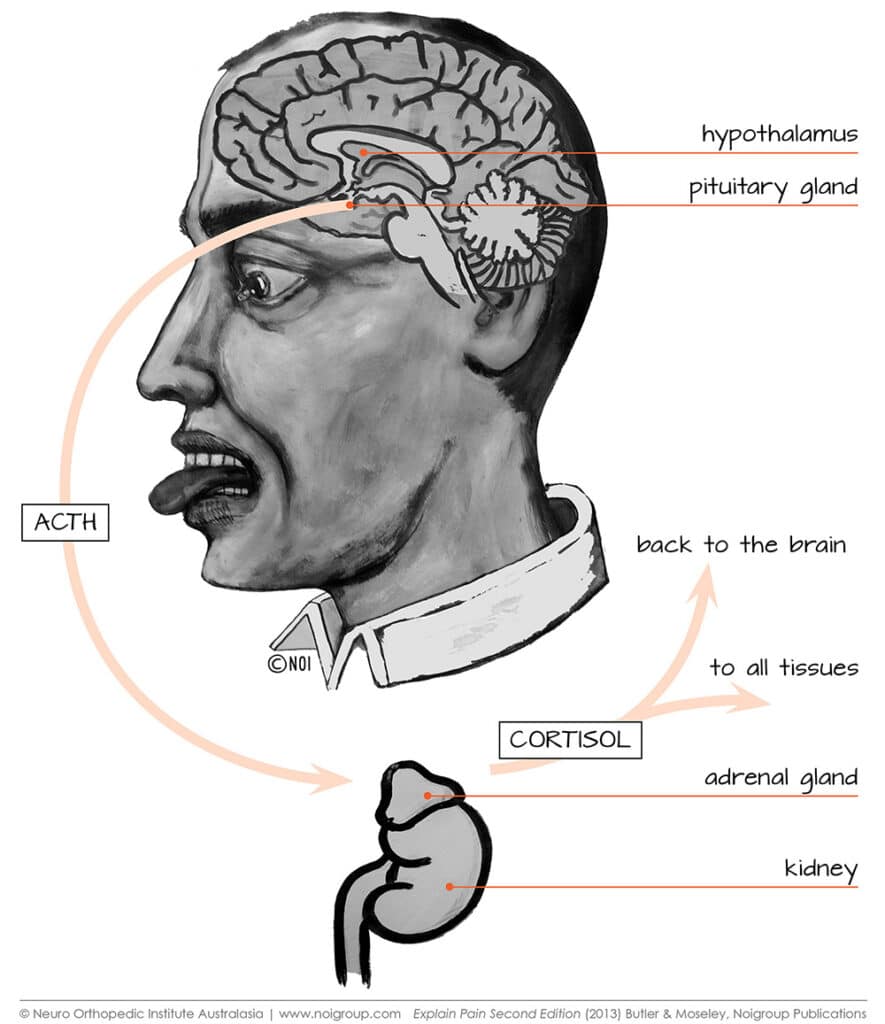
One key reason lies in the hypothalamic-pituitary-adrenal (HPA) axis – your body’s hormonal stress system, which regulates cortisol. This hormone affects nearly every tissue in your body. With repeated or prolonged stress, the HPA axis can become dysregulated, leading to altered inflammation, increased pain experience, and changes in the ability to modulate nociceptive input.
These systems are deeply connected: a chronic stress response – whether related to pain or other stressors – can initiate, exacerbate, or prolong the pain experience, and may interfere with recovery processes (Hannibal & Bishop, 2014). This is why stress shows up so consistently alongside conditions like fibromyalgia, chronic fatigue, and persistent musculoskeletal pain.
Some things make it harder to break the cycle
Certain experiences are particularly powerful in amplifying the stress response. If you’re living with persistent pain, you’re likely familiar with several of them: Unpredictability, loss of control, feeling isolated or unsupported, the creeping sense that things are getting worse rather than better. Each of these is associated with measurable changes in stress-related physiological activity.
What can we do?
There’s no single switch to flip. And you wouldn’t want to eliminate stress entirely – in the right amount, it’s one of your body’s most powerful catalysts for learning and adaptation. But you can influence how your body responds to it – and that’s where the #BeTheChange message becomes meaningful, and where small, consistent changes start to matter:
- Building supportive connections.
-
Creating more predictability in daily life where you can.
-
Consider how you can explore uncertainty safely when you’re up for it.
- Finding movement that feels manageable rather than punishing.
- Giving your body genuine recovery time.
Even modest changes, applied consistently, add up.
As a practitioner, when we say to a patient, ‘You need to slow down’ or ‘You need to move’, they may interpret this as they’re doing something wrong. The practitioner acknowledging that feeling can be a useful first step.
Sleep is worth a particular mention here. Research shows that disrupted sleep produces a low-grade inflammatory response that reduces your capacity to respond to stressors – which in turn affects pain (Wyns et al., 2023). If you’ve been told ‘Sleep is important’ and found that advice more frustrating than helpful, that’s understandable – the pressure to sleep well can itself become a source of stress. Structured rest, even when sleep feels out of reach, gives your nervous system a chance to shift out of a sustained stress response.
It’s also worth knowing that if someone in your care has told you to ‘slow down‘ or ‘keep moving‘ and it landed as criticism rather than support, that’s a common experience. How recommendations are framed matters. You’re not doing anything wrong by finding it hard.
A final thought
Stress isn’t the enemy. It reflects your body responding to challenge and it might be useful to view it as an opportunity to support a system that can respond and then recover.
In chronic pain, stress is rarely the whole story. But it’s often one of the most important and under-acknowledged parts of it. When you begin to understand what your body is actually doing – and why – something changes. Not necessarily the pain itself, at first, but your relationship to it.
That’s often where recovery can begin.
– The Noigroup Team
If you’d like dive deeper into the biology of stress, pain, and recovery, you are welcome to explore our courses (for clinicians) and resources (for clinicians and general public).
Further reading and references
Butler & Moseley – Explain Pain Second Edition (2013)
https://europeanpainfederation.eu/sip-news/april-is-stress-awareness-month-bethechange/
https://www.stress.org.uk/stress-awareness-month-2026/
https://www.preventivehealth.sa.gov.au/about/news-announcements/stress-awareness-month
https://www.noigroup.com/noijam/stressed-unstressed/
https://www.noigroup.com/noijam/glia-unsung-protector-in-pain/
https://www.noigroup.com/noijam/world-sleep-day-2024-how-does-sleep-and-pain-relate/
https://www.noigroup.com/noijam/extending-stress-into-the-body-but-what-about-the-world/
Robert Sapolsky – Why Zebras Don’t Get Ulcers
Hannibal, K. E., & Bishop, M. D. (2014). Chronic stress, cortisol dysfunction, and pain: a psychoneuroendocrine rationale for stress management in pain rehabilitation. Physical therapy, 94(12), 1816–1825. https://doi.org/10.2522/ptj.20130597
Wyns, A., Hendrix, J., Lahousse, A., De Bruyne, E., Nijs, J., Godderis, L., & Polli, A. (2023). The Biology of Stress Intolerance in Patients with Chronic Pain-State of the Art and Future Directions. Journal of clinical medicine, 12(6), 2245. https://doi.org/10.3390/jcm12062245

Loved the succinct yet full manner of the descriptions here. I did have to read it a few times to disconnect and reconnect my own knowledge filter around issues of stress and learning (the yeh buts) so it’d be great to know of any surveys of message impact you are doing in your work with people with chronic pain.