In this edition of Noijam, we’re exploring a complex piece of physiology that might help make sense of some of the odd changes in pain and sensory experiences. This one’s for people on their own journey with recovery who are curious and want to dive a little deeper into the physiology – and we hope clinicians may also find it a helpful gateway into the world of glia and the complex physiology of pain, especially if this is new territory. It’s worth noting that glia are just one piece of the puzzle when it comes to persistent pain, and this Noijam aims to explore just this one interesting piece.
A big thanks to Professor Mark Hutchinson for his review of this Noijam edition.
You may have heard about neurons – the nerve cells that ‘fire’ to send messages along the nervous system. What often surprises people is that neurons make up only a fraction of our nervous system. The majority of cells are remarkable immune‑like cells called glia – they’re actually far more common than neurons.
Glia (Greek for ‘glue’) were once thought to be just support crew, giving structure and scaffolding for the nervous system to do its work (He et al., 2007). But, around the turn of the 21st century, researchers showed that glial cells may actually be far more important than we first believed (Watkins et al., 2001; He et al., 2007). We now know these cells are active players in shaping how sensitive and responsive our nervous system is – including how potentially threatening sensory information from our body (such as inflammation, tissue change, or temperature shifts) is transmitted to higher levels of our central nervous system (including the brain) and processed.
Glial cells are found not just in the brain but in the spinal cord and along nerve pathways, and can be thought of as the surveillance officers of the nervous system – scanning the environment for molecules that may signal a threat to the organism. When they detect signs of injury, stress, infection, or emerging research suggests even psychological and social threats (Blank & Prinz, 2024), they release chemicals that help ramp up the body’s protection. You could think of this as one of the system’s volume dials, increasing the ease with which sensory information can be sent. This response is useful at first – it’s part of how we heal and stay safe.
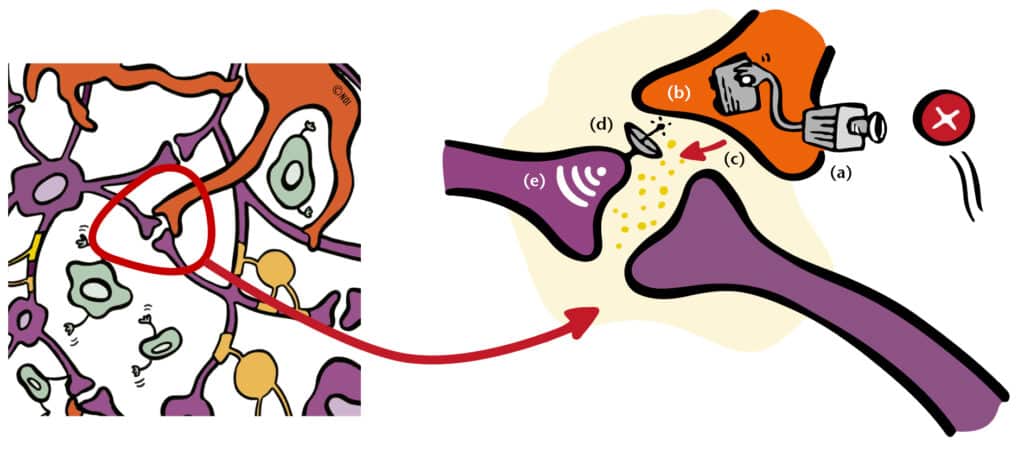
Figure. The purple cells are neurons, the ones that send messages through the nervous system. The orange cells are glia – immune-like cells that act as surveillance officers, constantly scanning for signs of potential threat to the body. This includes physical injury, long-term changes in stress hormones, or even signals related to psychological or social stress. When glia detect these molecular cues, they can ramp up the system’s sensitivity by turning up the ‘volume’ on neuron-to-neuron communication (as shown in the zoomed-in section). This helps us heal and stay safe in the short term – but may also contribute to persistent pain when the system stays sensitised. Image: Explain Pain Supercharged, Noigroup Publications, 2017.
But here’s the twist
Glia have a kind of neuroimmune memory (metaphorically speaking). The neuroimmune system, including glia, can become primed from previous threats (Grace et al., 2014). It isn’t conscious – it’s the system reinforcing connections that keep protective responses going. Have you ever noticed that once you’ve had a problem in one body area, it’s more likely to be the place where symptoms return or spread? That doesn’t necessarily mean there’s new or more damage – but we may have a volume dial that’s already primed (you could think of it like having more security cameras that are even more sensitive to detecting things going on in the yard). It could be that this neuroimmune system is doing its job of keeping you safe, even when it isn’t helpful for your recovery.
One of the key learning concepts many people report as powerful in their recovery journey is this: ‘I can retrain my overprotective pain system’ (Leake et al., 2021). Glial cells are just one part of the complex physiology underpinning this concept.
The good news?
These same glial networks that can keep our system alert can also change and decrease protection, given the right environment. Just like learning a skill, protective pathways can be pruned or reshaped – especially when we introduce the right mix of safety, challenge, novelty, movement, education, support, and meaningful connection. This might include graded movement, building confidence, understanding your pain story, reconnecting socially, or gradually returning to valued activities. There is even research exploring medicines that aim to decrease glial activity (Watkins et al., 2001; Donnelly et al., 2020).
In all, these may be strategies that help turn down the volume knob – but what helps nudge one person’s sensitivity can look very different to the next. It tells us that the key to moving forward may involve some novel and surprising strategies.
In fact, this is one of the reasons many people find tools like The Protectometer Handbook (or the Resolve Back Pain or Knee Osteoarthritis Handbook) so transformative – they aim to empower people to nudge the system toward safety, and trust in their body again. And this is why recovery from pain is never purely physical – our clever systems are responding to all the stressors and information in our world, not just the physical ones.
– Brendan Mouatt
References
- Blank, N., & Prinz, M. (2024). Mind the GAPS: Glia associated with psychological stress. Glia. https://doi.org/10.1002/glia.24521 (Open access via PubMed Central)
- Donnelly, C. R., Hensel, J. M., & Ji, R.‑R. (2020). Central nervous system targets: Glial cell mechanisms in pain. Neurotherapeutics, 17(1), 48–67. https://doi.org/10.1007/s13311-020-00905-7
- Grace, P. M., Hutchinson, M. R., Maier, S. F., & Watkins, L. R. (2014). Pathological pain and the neuroimmune interface. Nature Reviews Immunology, 14, 217–231. https://doi.org/10.1038/nri3621
- He, J., Sun, X., & Wang, Z. (2007). Glial cells are more than support cells? Neuroscience Bulletin, 23(1), 41–45.
- Leake, H. B., Moseley, G. L., Stanton, T. R., O’Hagan, E. T., & Heathcote, L. C. (2021). What do patients value learning about pain? A mixed-methods survey on the relevance of target concepts after pain science education. Pain, 162(10), 2558-2568.
- Watkins, L. R., Milligan, E. D., & Maier, S. F. (2001). Glial activation: A driving force for pathological pain. Trends in Neurosciences, 24(8), 450–455.

comments