
Mobilisation of the Nervous System to Mobilisation of the Neuroimmune System
I wrote Mobilisation of the Nervous System about a quarter of a century ago while working in a hospital in Dartford, Kent – I remember thinking that only my family would buy it. I still find it very humbling, but many people did buy it, and 25 years later, tens of thousands of participants have taken the MOTNS course. Although the course has been refreshed many times, it’s time for a major refresh – not just the name, but also the core underlying thinking and paradigms. This year, Michel Coppieters and I will run the first Mobilisation of the Neuroimmune System courses in Sydney and Adelaide, Australia.
What’s new?
The major refresh is to acknowledge and incorporate the immune system. In retrospect we should never have missed it. Of the trillion or so cells in the nervous system only about half are neurones, the other half are mostly glia; historically dismissed as literally ‘glue’ – as packing and support for the neurones. But most of this “other brain”, such as microglia, astrocytes and Schwann cells, have immune functions and an intimate reciprocal relationship with neurones – the brain hasn’t changed, it’s always been a neuroimmune organ – it’s our thinking that needed catching up. The neuroimmune system is a critical player in learning, memory, movement and sensitivity, and neuroimmune thinking demands a far wider view of neurodynamics.
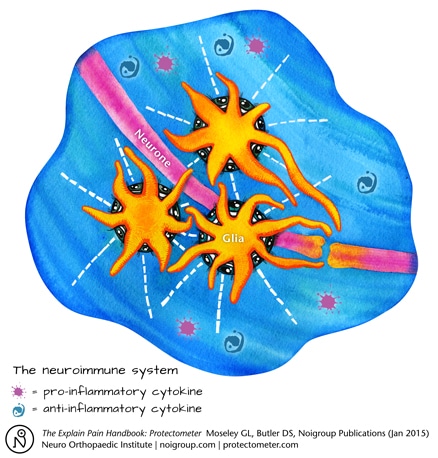
Another aspect of the refresh is one that is ongoing – taking on and incorporating the somewhat quieter but continuing, research into neurodynamics. Recent papers include Nee et al’s (2012) work, which demonstrates that neural mobilisation can be effective and safe for nerve-related neck and arm pain, or some emerging work which might question the notion of ‘musculoskeletal’ conditions such as ‘patellofemoral pain syndrome’ (Huang et al 2015).
But we mustn’t forget the quality of the old. For me, the two most comprehensive books on peripheral nerve problems are still Sunderland (1978) and Mumenthaler & Schliack (1991). They both reek of quality of clinical examination linked to research. Much of Sunderland’s work was carried out on soldiers post WWII. Sunderland helped me construct a science base for neurodynamics and I recall him saying that there was ‘no profession out there looking after the minor but often very painful peripheral nerve injuries’. Michel Coppieters work carries on this tradition and we look forward to featuring this in coming weeks on noijam.com.
Can you really move Schwann cells, microglia, astrocytes and oligodendrocytes?
You can – especially in peripheral nerves, cord and probably hindbrain. With my clinical science hat firmly on, I think it would be reasonable and sensible to suggest that associated connective tissues, the cells and the milieu probably enjoy a good wriggle, tease, and flush as part of their normal movement, especially when there is a bit of inflammatory soup around or fibroblasts needing a bit of polarisation (see Gilbert et al 2014 for some basic science support of this idea).
But embracing the immune system is much more than just the movement…
A Straight Leg Raise is antigenic
The term antigenic usually refers to a substance (pathogen) initiating an immune response. But movement (along with learning and thinking) can also initiate immune activity and thus can be called antigenic. A Straight Leg Raise (SLR) is a test of many things ranging from physical abilities of tissues in the leg, whether the owner of the leg likes the person lifting the leg, to how they perceive the quality of the elastic in their underwear. It is also a test of the precision and sensitivity of the neuroimmune architecture representing the movement and the meaning of the movement at that particular time. For example microglia and astrocytes in the brain and cord in their surveillance role repeatedly check for danger. If the SLR is deemed dangerous by the leg owner then the microglia and astrocytes may well contribute to modifying the brain representation of the SLR – including when the brain ‘decides’ it is safe to stop the movement.
The sensitivity of the movement will also likely be altered. At our recent Explain Pain 3 day course in Melbourne, Prof Bob Coghill spoke about ‘top down tuning’ of the peripheral nervous system and he provided a beautiful summary: ‘cognitive factors can powerfully shape the processing of afferent information, potentially through dynamic, task dependent tuning of afferent processing mechanisms’ – this really got us excited. To us, this suggests that not only can the meaning of a movement, in this case a SLR, have a neuroimmune effect on the brain, but the brain can then ‘tune’ the processing of incoming information in the periphery – thereby altering the messages the brain receives, which will then potentially influence cognition, which may have a further tuning effect and so on! Think of this next time you lift someone’s leg in the air! A ‘simple’ SLR doesn’t seem so simple anymore!
Whew!
We clearly have to be smarter at doing our active and passive neural mobilisations and adopt a much broader neuroimmune paradigm in our clinical reasoning. So much of this relates to the idea of context and meaning, and drawing the immune system in adds the notion of ‘self’ and neuroimmune responses to perceived danger to this ‘self’ – can you see how this might influence the range, quality and experience of a SLR depending on whether it is ‘self or ‘other’ doing the moving? Our assessment, intervention and education skills related to any sensitivity and stickiness exhibited when we move the nervous system can be refined and sharpened by this overdue integration of the immune system.
A final juicy morsel
The word ‘mobilise’ is often thought of as just meaning ‘move’. But mobilise has a broader meaning too – ‘to make ready for movement’, ‘to assemble or prepare something in response to need’ and to ‘liberate or excite quiescent material to physiologic activity’. These rich ideas are all incorporated into mobilising the neuroimmune system.
David Butler
Mobilisation of the Neuroimmune System is coming! Based on the latest evidence, the Mobilisation of the Nervous System course has been updated and re-written ‘from the basic science up’, integrating the neuroimmune system as a critical player in learning, memory, movement and sensitivity. The MONIS course provides a clinical reasoning framework to identify those patients who will benefit from neurodynamic mobilisation and the essential practical skills to examine and manage the physical health of the nervous system. Adelaide 24-25 July and Sydney 1-2 August 2015
References
Gilbert KK et al. (2014). Effects of simulated neural mobilization of fluid movement in cadaveric peripheral nerve sections: implications for the treatment of neuropathic pain and dysfunction. Journal of Manual and Manipulative Therapy. DOI: 10.1179/2042618614Y.0000000094.
Huang B-Y et al (2015). Predictors for identifying patients with patellofemoral pain syndrome responding to femoral nerve mobilization. Archives of Physical Medicine and Rehabilitation. DOI:10.1016/j.apmr.2015.01.001.
Mumenthaler, M. and H. Schliack (1991). Peripheral Nerve Lesions. New York, Thieme.
Nee RJ et al. (2012). Neural tissue management provides immediate clinically relevant benefits without harmful effects for patients with nerve-related neck and arm pain: a randomised trial. Journal of Physiotherapy 58(1) pp 23-31.
Sunderland S. (1978) Nerves and nerve injuries. 2nd ed. Baltimore: Williams and Wilkins.

Interesting article
http://www.nationalgeographic.com/healing-soldiers/blast-force.html
I have to say that I really appreciate your “new” way of thinking ;-). Not long after being diagnosed with CRPS, I needed to see a physio for shoulder and neck issues caused by walking aides etc. Leanne, the physio, pointed out very gently, how some movements even very small, could affect the nerves in my foot quite badly if I was correctly prepared for the movements. We have the ability to damage ourselves so easily.
Hi there,
Thanks – I would like to add that part of the “new way” of thinking is the awareness that it is very hard to damage nerves and other tissues in a CRPS affected body part. The brain, acting on the best evidence available develops such a protective sensitivity via neuroimmune interactions that it is almost impossible to damage anything by movement. Sorting out and dealing with the reasons why the brain constructed such protective sensitivity is an essential part of CRPS treatment.
Best wishes
David
First of all David , thanks for your continued work. If I could throw some of my swirling thoughts into the cauldron for unravelling – Patients with alleged FMS and pain all over ,who are also hypothyroid , with low immunity due to hypothyroidism ( possibly untreated, see stop the thyroid madness) . If thyroxine is one of the drivers of cell function then it will affect the way in which the nerves function and hence pain. This sounds a bit simplistic but we are using “sticking plaster ” treatments instead of looking at the cause which I am beginning to think is physiological more than mechanical.
Reblogged this on alignment ba and commented:
Interesting read
Hi – thanks for this email. It was a pleasure to read. I am a Pelvic Physio, and would LOVE some idea on ASSESSING and TREATING the Nerves of the Pelvis, particularly Pudendal, Genitofemoral, iliohypogastric & Ilioinguinal. I find it frustrating to not have anything but palpation (sometimes with Pudendal), and subjective info to go on for many of these important nerves. Would your Sydney based course cover these nerves? If so I will be there. Would love to know your thoughts here. Thanks in advance. AJ
Hi Ange,
Many thanks for your note. I have looked for hints of altered mechanical abilities in these nerves for many years and I think it is not that common unless there is some local trauma/surgery. My clinical suggestion is that perhaps the obturator and lateral femoral cutaneous nerve may be physically involved more. For the nerves you have listed, hip extension and testing combinations of abduction/adduction and hip rotation may pick up a sticky or stuck anterior hip nerve. There is no formal pudendal nerve biomechanics that I am aware of but squatting and SLR would surely load it.
Most current pelvic pain physiotherapy seems very biomechanical to me. We are aware that peripheral nerves can upregulate, for example high threshold fibres may behave more like low threshold fibres, cell bodies in DRGs upregulate as well and fibres may become adrenosensitive among other adaptations. I guess if a person “deems” that their pelvic area needs protection, then peripheral nerve changes are just one of the many processes available. But what this means is that the nerves may still move and slither around quite nicely, ie sensitive but still mobile.
There won’t be much specific on the IH,II and GF nerves in the course though they will be covered. There will be heaps more about peripheral nerve sensitisation and what we can do about it with movement education, imagery etc.
Happy to chat on further about this
Cheers
David
Im following the “neuro” unfolding story with keen interest.
Iv been a Rolfer for 45 years, following my initial sessions with IdanRolf herself. I was inspired by the positive results in my structure. My question is; are you suggesting we abandon manual therapy, and the ideas and techniques that have apparently served so well? Do you advocate dropping these approaches entirely? If not can you speak to integration of this “neuro” material into daily practice? Jan
Hi Jan,
There is no suggestion of abandoning manual therapy, only making it richer.
Best wishes
David