I was really struck by the coincidence of reading in the same week that Bob Elvey had passed away, and that Bob Nee, Michel Coppieters and their team (Bill Vicenzino, Gwen Jull, and Josh Cleland) had won the prestigious Journal of Physiotherapy ‘Paper of the Year’ award with a randomised controlled trial that included ‘Elvey techniques’ (Nee et al. 2012).
I didn’t know Bob Elvey well; we only met 3 or 4 times, shared a few beers at conferences and I subscribe to the general consensus of a ‘damn good bloke’. Early on in my career, I read everything I could about his pioneering work with the Upper Limb Neurodynamic Test and his novel management strategies for patients with neuropathic pain. His death stimulated me to reread his papers in old proceedings from Manipulative Physiotherapy Association of Australia symposia in from the 70s and 80s. These were the days when clinicians ruled the roost and I still think these symposia were full of great thinking! Bob always reinforced attention to handling skills, reasoning and, somewhat unique for the time, he always questioned what might be happening physiologically. It was ‘out there’ stuff.
Some 30 plus years later, Bob Nee et al. used a parcel of interventions in their clinical trial on 60 patients with nerve related neck and arm pain. The parcel included de-threatening education (albeit brief), nerve mobilisation using ‘sliders’ and ‘tensioners’, as well as some ‘Elvey techniques’. For details of the study protocol, something I would recommend for any young researcher, please read Nee et al. (2011).
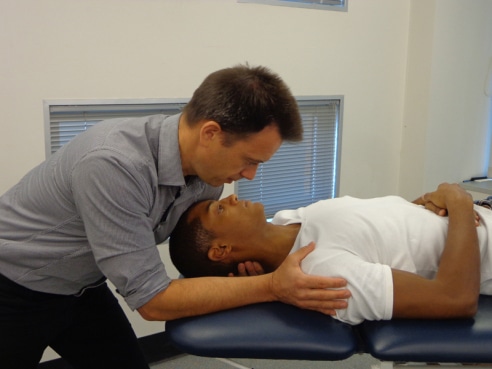
In the image you can see the elegant Michel Coppieters performing one of Elvey’s techniques (a cervical contralateral lateral glide mobilisation). From the base position shown, the neck (either with or without the cranial cervical segments and head) is translated (no rotation or lateral flexion) away from the sore side. The technique can be applied to specific levels, for example C4-C5. The mobilisation can also be performed with the elbow extended to preload the nervous system. Note that this is an attempt to mobilise structures around the nervous system, rather than a direct nervous system mobilisation. The technique is well described (Nee et al. 2011) and has previously shown beneficial effects (Allison et al. 2002, Coppieters et al. 2003). Other techniques recommended by Bob Elvey involve oscillatory shoulder girdle depression while gently abducting the arm, or combining a lateral glide of the neck away from the painful side with mobilisation of the shoulder girdle (as in sliding or tensioning techniques).
In the clinical trial, symptoms were not provoked during treatment. Techniques were performed so that participants only felt a gentle stretching or pulling sensation.
Following four sessions and a home exercise program, 53% of participants in the treatment group had improved compared to only 15% of participants in the advice to remain active control group (ie, a number needed to treat (NNT) between 2 and 3).
Nee et al. concluded that “these results enable physiotherapists to inform patients that neural tissue management provides immediate clinically relevant benefits (…) with no evidence of harmful effects”. Simply said ‘it works’. I think the finding of “no evidence of harmful effects” when performed by skilled clinicians is even more powerful. I know some practitioners are wary of mobilising the nervous system, but I am already aware from my post graduate student discussion sites of practitioners now handling patients far more confidently since this research emerged.
I think Bob Elvey would have predicted and surely been delighted with the results of the Nee et al. study. Although I believe we should never use surnames to refer to techniques, in this blog I happily make an exception and refer to the techniques as ‘Elvey techniques’ as a tribute to one of physiotherapy’s greatest.
Allison, G. T., B. M. Nagy, and T. Hall. 2002. A randomised clinical trial of manual therapy for cervico-brachial pain syndrome- a pilot study. Manual Therapy 7:95-102.
Coppieters, M. W., K. H. Stappaerts, L. L. Wouters, and K. Janssens. 2003. The immediate effects of a cervical lateral glide treatment technique in patients with neurogenic cervicobrachial pain Journal of Orthopaedic and Sports Physical Therapy 33:369-378.
Nee, R. J., B. Vincenzino, G. A. Jull, J. A. Cleland, and M. W. Copieters. 2011. A novel protocol to develop a prediction model that identifies patients with nerve related neck and arm pain who benefit from the early introduction of neural tissue management Contemporary Clinical Trials 32:760-770.
Nee, R. J., B. Vincenzino, G. A. Jull, J. A. Cleland, and M. W. Coppieters. 2012. Neural tissue management provides immediate clinically relevant benefits without harmful effects for patietns with nerve-related neck and arm pain: a randomised trial. Journal of Physiotherapy 58:23-31.
– David Butler
www.noigroup.com

I saw Bob Nee present at the IFOMPY conference in Vail in the ’92. He began by playing a video of violent Aussie Rules football accompanied by furious rock music; stopping it suddenly and proceeding to speak. It was riveting, and I always thought this represented the two sides of manual care, his being the far gentler one. I’ve seen many speakers, most forgettable. I never forgot Elvey.
This Noijam reminded me of a paper I read as a new grad from Bill Vicenzino and I have dug it up to demonstrate how we have moved along in 10 years!
(Vincencino. B. Lateral epicondylalgia: a musculoskeletal physiotherapy perspective. Manual Therapy (2003) 8(2), 66–79)
A “masterclass” on treatment of LE (for the time) and interestingly discusses the use of the Elvy cervical contralateral lateral glide mobilisation. At the time, I can remember being amazed by the immediate improvement in P1 grip strength (first instance of pain on grip dynamometer) immediately after 30-60 seconds of repetitive gliding. Without touching the elbow at all!
I remember it becoming quite clear to me from this test that LE was obviously a more complex process than purely an overuse injury involving the wrist extensors and supinators. A great way to also demonstrate and educate sufferers on the importance of nerve tissue management in the treatment program (whether you call them glides, slides or nerve “flossing”!)
Don’t believe me? No harm in giving it a go next time a budding Pat Rafter wanders into your clinic!
Cheers
Hi Christopher
Yes – I found that observation to be fascinating as an early career physiotherapist when I had the privilege of working with Bob in his practice. We used it quite a bit during the RSI period in WA. It obviously left an impression – then using it in clinic and including it in my paper.
So yes, it is something that might be a nice adjunct to help someone over the acute phase as you imply. The duration of that effect was then dependent on many factors – as you would appreciate as a NOI follower.
As a somewhat related aside that you might find interesting: an observation I noted from a number of our studies on tennis elbow (note that we excluded concomitant neck and upper limb symptoms that interfered with ADL etc) was that PPT at the elbow underwent substantially greater improvements with the LV technique compared to the elbow MWM, whereas the opposite was the case for PFG.
bill
I’ve always wondered, is treating the neck in tennis elbow more about DNIC and bamboozling the patient than we think?
I was always told when i was training to “clear the neck” i’m still not sure what that actually means.
hi Dave
Agree with you regarding the clear the neck statement – it can be confusing to precisely define (in research as well as clinic) what that means?
Not so sure I agree with your comment on DNIC: because by definition involves a noxious stimulus and the LV technique is usually applied in a way that it is not painful, so probably not likely a plausible mechanism. Hopefully that refines your conceptualization a bit?
bill
I am intrigued here by the possible biological modes of effect of the treatment intervention. Take the hands on translation technique. I believe it is important and concur with Bill V about its effects in the clinic with the overuse syndrome group. Elvey inspired techniques like this at least gave us a foothold in the RSI epidemic back in the 80s, when in retrospect we really didn’t have much of a clue what was going on!
But what might this technique do to physiology. (Note that it is quite hard to do to yourself). Maybe the technique is all about:
– skillful “knowing” hands on “feeling the problem” and thus dethreatening.
– a novel movement away from the problem side.
– a movement which can be shown to have immediate benefits but empowered by linking it to something the patient can do themselves (slider/tensioner homework).
– a movement signalling resident and remote glial cells not to be on so much guard – A kind of “it’s alright look what the neck can do now”
– meningeal and local CSF mobilisation. Remember nerve roots get at least half their nutrition from CSF. CSF probably gets a bit stagnant in the little pockets around the nerve roots in a neck that hasn’t moved properly for a while.
– a vascular and neural tissue agitation and flush out (terribly scientific!) – just doing what they are designed to do anyway.
Maybe just the education and home exercises would have had the same effect, somehow I don’t think so.
David
Thanks very much David for highlighting our study in this tribute to Bob Elvey.
Finding a way to answer the question about potential mechanisms behind the observed treatment effect is always complex. Your last statement emphasizes an important point about interpreting the results of our study. Given that brief education, manual therapy with the ‘Elvey techniques’, and the home program of ‘sliders/tensioners’ were applied as a package for all participants, we don’t know whether only certain parts of the package are needed to achieve the observed effects or whether the entire package is necessary.
An obvious next step would be to perform future trials to determine how much each part of the package contributes to treatment effects (eg, are education, ‘Elvey techniques’, and home exercises really superior to just education and home exercises?). However, some researchers, clinical trial funding agencies, clinicians, and patients might feel it is a higher priority to find out how the package used in our trial compares to other ‘treatment packages’ that could be appropriate for this group of patients.
Cheers,
Bob Nee
Yes, yes and yes again all the above David. By the way Bob was a lovely man and he always said of himself ” What you see is what you get” What you got was magic at the time and hey a little magic in the practice can work wonders. Like Geoff Maitland and others of his era he gave us broad shoulders to stand on…..
well put – couldn’t agree more – the likes of Bob and Geoff indeed set a platform for many of us to build upon – for that I am extremely grateful
I’d like to ask people here. In the context of neural management interventions and immediate treatment effects (within session changes), do you suspect the primary mechanism of effectiveness to be a) an actual reduction in peripheral neural tissue mechanosensitivity ( direct change in synaptic thresholds), or b) a reduction in perceived threat by the CNS ( the CNS takes in peripheral somatosensory frequencies and in combination with cognitive-evaluative and affective processing a top down regulation of nociceptive drive is created )? Would it be a mistake to separate these two processes in trying to conceptualize mechanisms of effectiveness of our interventions? Option b is context sensitive and makes more sense to me. Option a assumes that the “cause of pain” is the mechanosensitivity of specific nerves that need to be identified and treated. If this was true, then we’d have to be very lucky to help patients improve. On the contrary, many different interventions seem to have the capacity to work. Thoughts?
references
http://www.ncbi.nlm.nih.gov/pubmed/20710090
http://onlinelibrary.wiley.com/doi/10.1002/wcs.1201/full
We are doing our best to break away from dualistic thinking so why can’t it be both, and…….when reflecting on the “and” lets not forget us – the practitioner and the patient – as beings, placing spirituality in the mix, that “magic ingredient”. My Dad, a physiotherapist bless him was a dinosaur as far as todays knowledge goes but wow what a big personality and what a huge shadow he cast ( I’ve been watching too many Rocky movies! ). I think if we were to compare our success rates of him then and me today I don’t think I’d be ahead……..the knowledge we have now is fantastic and we are living in exciting times for our profession. I know the new science has revitalised me, after so many years as a physiotherapist however, in my opinion the application is an Art. Lets not loose the patient in the mix……
Hi Evan and David,
I don’t think it can be separated and I suspect that Nee et al included interventions more likely to target peripheral change (eg hands on technique) and intervention more likely to target central changes (eg education).
The old peripheral/central dualism is hopefully going, though strongly anchored by language (eg peripheral nerve, central sensitisation). Even the concept of central immune privilige which helped strengthen the dualism is weakening as we know that nerve injury, similar to the kind treated in the Nee et al study, is likely to lead to altered blood/cord and blood/brain barriers.
I could think of a number of more peripheral pathophysiology (eg increased endoneurial fluid pressure) and more central pathophysiology (fear based neurosignatures) which the techniques arguably addressed. I don’t think peripheral and central pathologies exist in isolation.
David
I was lucky enough to be a postgraduate student of Bob’s and he was an inspiration to watch. It was if he was listening to the tissues for their response, adapting and inventing as he went along. His teachings were more about what he didn’t say than the actions he took. He was not so interested in the anatomical cause of the pain but providing comfort to the patient. This agrees totally with your discussion on the need to remove the dualism that exists and indeed rediscover the magic. In the not too distant future that ‘magic’ will be understood.