Terrific interview with Michael Salter at the Pain Research Forum. A brief bio from the site:

Michael Salter, MD, PhD, is chief of research at The Hospital for Sick Children (SickKids), a senior scientist in the Program in Neurosciences & Mental Health, and a professor of physiology at the University of Toronto, Canada. Salter’s main research focus is on synaptic physiology, in particular in relation to pain, and his work has led to new paradigms about neuroplasticity and how synaptic transmission in the central nervous system is regulated by biochemical processes within neurons and by glial-neuronal interactions.
Some highlights from the conversation (questions from the PRF in bold, answers in italics)
“You work on microglia and sex differences now. Why did it take so long for people to recognize how important microglia are?
It’s not just microglia that were relegated to second-class citizens—it was the whole area of glia. For the history of neuroscience, the major focus, and maybe rightly so, has been on neurons—on the electrically excitable cells, or at least cells that you could envisage being electrically excitable. This goes all the way back to Galvani and his experiments with the frog leg; you could stimulate the leg electrically and it moves. Obviously, it’s the electrical transmission of information that’s important.
So one can understand why there was this focus on neurons. Then, Virchow had the idea that the non-neuronal elements—the glia—were like glue. “Glia” is actually Greek for “glue.” It’s like thinking about the bricks and mortar in your house. Some people are interested in that, but most people are interested in what goes on in the house. That was part of the reason that glia had been largely ignored. But we now know that glia are much more than just glue!
Where is the microglia field headed? Is there a lot of hype?
The subtleties of microglial signaling are really starting to become apparent, so it’s not hype. But undoubtedly we’re in this rising phase where there will be enhanced expectations and perhaps some misunderstanding. For instance, there’s still this persistent misconception that microglial cells are either on or off. But they’re on all the time in their normal surveillance mode.
The way I think about these cells is that they can adapt in a variety of different ways, some of which are quite easily seen by changes in the number of the cells or their morphology. But there are other, probably more subtle ways the cells can be involved in physiological or even pathological changes that you might not see if you just look at morphology.
We’re now really trying to understand how signals the microglia receive are interpreted, processed, and how those cells communicate with neurons, astrocytes, and other cells. I think we haven’t hit the peak yet, but undoubtedly it will go up, and then come back down to some steady-state level.”
According to Google Scholar, Michael Salter has published hundreds of papers which have been cited over 26,000 times. Together with Simon Beggs from UCL, he has written some cracking papers, here are just two (both titles linked to open access papers) that you should know about
Microglia-neuronal signalling in neuropathic pain hypersensitivity 2.0
Microglia are increasingly recognized as critical in the pathogenesis of pain hypersensitivity caused by injury to peripheral nerves. The core signalling pathway is through P2X4 purinergic receptors on the microglia which, via the release brain derived neurotrophic factor, cause disinhibition of nociceptive dorsal horn neurons by raising intracellular chloride levels. This disinhibition works in synergy with enhanced excitatory synaptic transmission in the dorsal horn to transform the output of the nociceptive network. There is increased discharge output, unmasking of responses to innocuous peripheral inputs, and spontaneous activity in neurons that otherwise only signal nociception. Together the changes caused by microglia-neuron signalling may account for the main symptoms neuropathic pain in humans.
(emphasis added to highlight a very nicely written statement…)
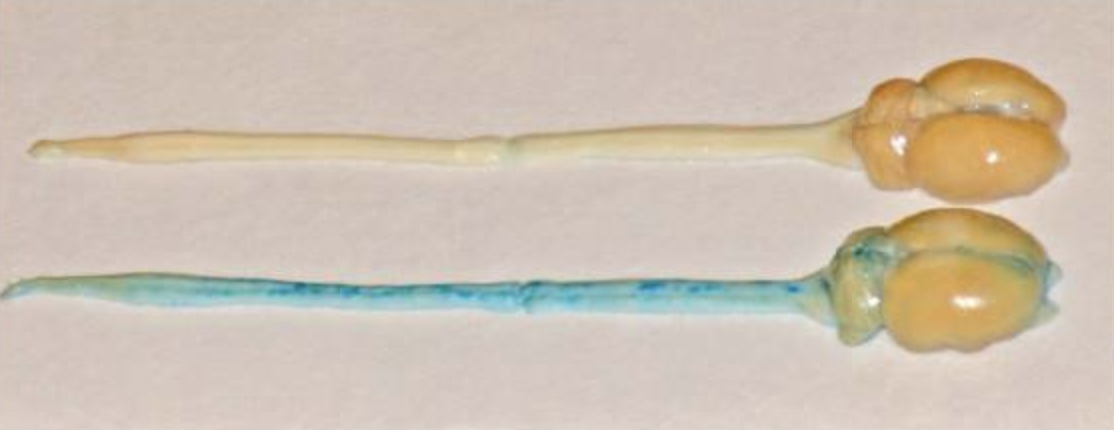
Peripheral nerve injury and TRPV1-expressing primary afferent C-fibers cause opening of the blood-brain barrier
We have discovered that injury to a peripheral nerve and electrical stimulation of C-fibers each cause an increase in the permeability of the BSCB and the BBB. The increase in permeability is delayed in onset, peaks at about 24 hours and is dependent upon action potential propagation. As the increase is mimicked by applying capsaicin to the nerve, the most parsimonious explanation for our findings is that the increase in permeability is mediated by activation of TRPV1-expressing primary sensory neurons. Our findings may be relevant to the development of pain and neuroplastic changes in the CNS following nerve injury. In addition, our findings may provide the basis for developing methods to purposefully open the BBB when needed to increase brain penetration of therapeutic agents that might normally be excluded by an intact BBB.
Happy reading.
-Tim Cocks

comments